BRUKINSA
These highlights do not include all the information needed to use BRUKINSA safely and effectively. See full prescribing information for BRUKINSA. BRUKINSA (zanubrutinib) capsules, for oral useInitial U.S. Approval: 2019
3e08fe23-d70e-424c-bc51-1222e320f902
HUMAN PRESCRIPTION DRUG LABEL
Mar 8, 2024
BEIGENE USA, INC.
DUNS: 081210042
Products 1
Detailed information about drug products covered under this FDA approval, including NDC codes, dosage forms, ingredients, and administration routes.
zanubrutinib
Product Details
FDA regulatory identification and product classification information
FDA Identifiers
Product Classification
Product Specifications
INGREDIENTS (9)
Drug Labeling Information
PACKAGE LABEL.PRINCIPAL DISPLAY PANEL
PRINCIPAL DISPLAY PANEL - 80 mg Capsule Carton
NDC 72579-011-02
Rx only
Brukinsa®
zanubrutinib
capsules
80 mg
Swallow capsules whole.
Do not open, break or
chew the capsules.
120 capsules
CONTRAINDICATIONS SECTION
4 CONTRAINDICATIONS
None.
None. (4)
WARNINGS AND PRECAUTIONS SECTION
5 WARNINGS AND PRECAUTIONS
5.1 Hemorrhage
Fatal and serious hemorrhage has occurred in patients with hematological malignancies treated with BRUKINSA. Grade 3 or higher hemorrhage including intracranial and gastrointestinal hemorrhage, hematuria, and hemothorax was reported in 3.8% of patients treated with BRUKINSA in clinical trials, with fatalities occurring in 0.2% of patients. Bleeding of any grade, excluding purpura and petechiae, occurred in 32% of patients.
Bleeding has occurred in patients with and without concomitant antiplatelet or anticoagulation therapy. Coadministration of BRUKINSA with antiplatelet or anticoagulant medications may further increase the risk of hemorrhage.
Monitor for signs and symptoms of bleeding. Discontinue BRUKINSA if intracranial hemorrhage of any grade occurs. Consider the benefit-risk of withholding BRUKINSA for 3-7 days before and after surgery depending upon the type of surgery and the risk of bleeding.
5.2 Infections
Fatal and serious infections (including bacterial, viral, or fungal infections) and opportunistic infections have occurred in patients with hematological malignancies treated with BRUKINSA. Grade 3 or higher infections occurred in 26% of patients, most commonly pneumonia (7.9%), with fatal infections occurring in 3.2% of patients. Infections due to hepatitis B virus (HBV) reactivation have occurred.
Consider prophylaxis for herpes simplex virus, pneumocystis jirovecii pneumonia, and other infections according to standard of care in patients who are at increased risk for infections. Monitor and evaluate patients for fever or other signs and symptoms of infection and treat appropriately.
5.3 Cytopenias
Grade 3 or 4 cytopenias, including neutropenia (21%), thrombocytopenia (8%), and anemia (8%) based on laboratory measurements, developed in patients treated with BRUKINSA [see Adverse Reactions (6.1)]. Grade 4 neutropenia occurred in 10% of patients, and Grade 4 thrombocytopenia occurred in 2.5% of patients.
Monitor complete blood counts regularly during treatment and interrupt treatment, reduce the dose, or discontinue treatment as warranted [see Dosage and Administration (2.4)]. Treat using growth factor or transfusions, as needed.
5.4 Second Primary Malignancies
Second primary malignancies, including non-skin carcinoma, have occurred in 14% of patients treated with BRUKINSA. The most frequent second primary malignancy was non-melanoma skin cancers (8%), followed by other solid tumors in 7% of the patients (including melanoma in 1% of patients) and hematologic malignancies (0.7%). Advise patients to use sun protection and monitor patients for the development of second primary malignancies.
5.5 Cardiac Arrhythmias
Serious cardiac arrhythmias have occurred in patients treated with BRUKINSA. Atrial fibrillation and atrial flutter were reported in 4.4% of patients treated with BRUKINSA, including Grade 3 or higher cases in 1.9% of patients. Patients with cardiac risk factors, hypertension, and acute infections may be at increased risk. Grade 3 or higher ventricular arrhythmias were reported in 0.3% of patients.
Monitor for signs and symptoms of cardiac arrhythmias (e.g., palpitations, dizziness, syncope, dyspnea, chest discomfort), manage appropriately [see Dosage and Administration (2.4)], and consider the risks and benefits of continued BRUKINSA treatment.
5.6 Embryo-Fetal Toxicity
Based on findings in animals, BRUKINSA can cause fetal harm when administered to a pregnant woman. Administration of zanubrutinib to pregnant rats during the period of organogenesis caused embryo-fetal toxicity, including malformations at exposures that were 5 times higher than those reported in patients at the recommended dose of 160 mg twice daily. Advise women to avoid becoming pregnant while taking BRUKINSA and for 1 week after the last dose. Advise men to avoid fathering a child during treatment and for 1 week after the last dose. If this drug is used during pregnancy, or if the patient becomes pregnant while taking this drug, the patient should be apprised of the potential hazard to a fetus [see Use in Specific Populations (8.1)].
- Hemorrhage: Monitor for bleeding and manage appropriately. (5.1)
- Infections: Monitor patients for signs and symptoms of infection, including opportunistic infections, and treat as needed. (5.2)
- Cytopenias: Monitor complete blood counts during treatment. (5.3)
- Second Primary Malignancies: Other malignancies have developed including skin cancers and non-skin carcinomas. Monitor and advise patients to use sun protection. (5.4)
- Cardiac Arrhythmias: Monitor for signs and symptoms of arrhythmias and manage appropriately. (5.5)
- Embryo-Fetal Toxicity: Can cause fetal harm. Advise women of the potential risk to a fetus and to use effective contraception. (5.6)
DRUG INTERACTIONS SECTION
7 DRUG INTERACTIONS
7.1 Effect of Other Drugs on BRUKINSA
Table 17: Drug Interactions that Affect Zanubrutinib|
Moderate and Strong CYP3A Inhibitors | |
|
Clinical Impact |
|
|
Prevention or management |
|
|
Moderate and Strong CYP3A Inducers | |
|
Clinical Impact |
|
|
Prevention or management |
|
- CYP3A Inhibitors: Modify BRUKINSA dose with moderate or strong CYP3A inhibitors as described. (2.3, 7.1)
- CYP3A Inducers: Avoid coadministration with strong or moderate CYP3A inducers. Dose adjustment may be recommended with moderate CYP3A inducers. (2.3, 7.1)
RECENT MAJOR CHANGES SECTION
RECENT MAJOR CHANGES
|
Indications and Usage (1.5) |
3/2024 |
DOSAGE & ADMINISTRATION SECTION
2 DOSAGE AND ADMINISTRATION
2.1 Recommended Dosage
The recommended dosage of BRUKINSA for monotherapy or in combination with obinutuzumab is 160 mg taken orally twice daily or 320 mg taken orally once daily until disease progression or unacceptable toxicity.
BRUKINSA can be taken with or without food. Advise patients to swallow capsules whole with water. Advise patients not to open, break, or chew the capsules. If a dose of BRUKINSA is missed, it should be taken as soon as possible on the same day with a return to the normal schedule the following day.
2.2 Dosage Modification for Use in Hepatic Impairment
The recommended dosage of BRUKINSA for patients with severe hepatic impairment is 80 mg orally twice daily [see Use in Specific Populations (8.7) and Clinical Pharmacology (12.3)].
2.3 Dosage Modifications for Drug Interactions
Recommended dosage modifications of BRUKINSA for drug interactions are provided in Table 1 [see Drug Interactions (7.1)].
Table 1: Dosage Modifications for Use with CYP3A Inhibitors or Inducers|
Coadministered Drug |
Recommended BRUKINSA Dosage |
|---|---|
| |
|
Clarithromycin 250 mg twice daily* |
80 mg twice daily† |
|
Clarithromycin 500 mg twice daily |
80 mg once daily† |
|
Posaconazole suspension 100 mg once daily |
80 mg twice daily† |
|
Posaconazole suspension dosage higher than 100 mg once daily Posaconazole
delayed-release tablets 300 mg once daily |
80 mg once daily† |
|
Other strong CYP3A inhibitor |
80 mg once daily† |
|
Moderate CYP3A inhibitor |
80 mg twice daily† |
|
Strong CYP3A inducer |
Avoid concomitant use. |
|
Moderate CYP3A inducer |
Avoid concomitant use. |
After discontinuation of a CYP3A inhibitor or moderate CYP3A inducer, resume previous dose of BRUKINSA [see Dosage and Administration (2.1,2.2) and Drug Interactions (7.1)].
2.4 Dosage Modifications for Adverse Reactions
Recommended dosage modifications of BRUKINSA for Grade 3 or higher adverse reactions are provided in Table 2.
Table 2: Recommended Dosage Modifications for Adverse Reaction|
Adverse Reaction |
Adverse Reaction Occurrence |
Dosage Modification |
|---|---|---|
| ||
|
Hematological toxicities[see Warnings and Precautions (5.3)] | ||
|
Grade 3 or Grade 4 febrile neutropenia Platelet count decreased to 25,000-50,000/mm3 with significant bleeding Neutrophil count decreased to <500/mm3 (lasting more than 10 consecutive days) Platelet count decreased to <25,000/mm3 (lasting more than 10 consecutive days) |
First |
Interrupt BRUKINSA |
|
Second |
Interrupt BRUKINSA | |
|
Third |
Interrupt BRUKINSA | |
|
Fourth |
Discontinue BRUKINSA | |
|
Non-hematological toxicities[see Warnings and Precautions (5.5) and Adverse Reactions (6.1)] | ||
|
Severe or life-threatening non-hematological toxicities* |
First |
Interrupt BRUKINSA |
|
Second |
Interrupt BRUKINSA | |
|
Third |
Interrupt BRUKINSA | |
|
Fourth |
Discontinue BRUKINSA |
Asymptomatic lymphocytosis in CLL and MCL should not be regarded as an adverse reaction, and these patients should continue taking BRUKINSA.
Refer to the obinutuzumab prescribing information for management of obinutuzumab toxicities.
- Recommended dosage: 160 mg orally twice daily or 320 mg orally once daily; swallow whole with water and with or without food. (2.1)
- Reduce BRUKINSA dose in patients with severe hepatic impairment. (2.2, 8.7)
- Advise patients not to open, break, or chew capsules. (2.1)
- Manage toxicity using treatment interruption, dose reduction, or discontinuation. (2.4)
DOSAGE FORMS & STRENGTHS SECTION
3 DOSAGE FORMS AND STRENGTHS
Capsules: Each 80 mg capsule is a size 0, white to off-white opaque capsule marked with "ZANU 80" in black ink.
Capsules: 80 mg. (3)
USE IN SPECIFIC POPULATIONS SECTION
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Risk Summary
Based on findings in animals, BRUKINSA can cause fetal harm when administered to pregnant women. There are no available data on BRUKINSA use in pregnant women to evaluate for a drug-associated risk of major birth defects, miscarriage, or adverse maternal or fetal outcomes. In animal reproduction studies, oral administration of zanubrutinib to pregnant rats during the period of organogenesis was associated with fetal heart malformation at approximately 5-fold human exposures (see Data). Women should be advised to avoid pregnancy while taking BRUKINSA. If BRUKINSA is used during pregnancy, or if the patient becomes pregnant while taking BRUKINSA, the patient should be apprised of the potential hazard to the fetus.
The estimated background risk of major birth defects and miscarriage for the indicated population is unknown. All pregnancies have a background risk of birth defect, loss, or other adverse outcomes. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2% to 4% and 15% to 20%, respectively.
Data
Animal Data
Embryo-fetal development toxicity studies were conducted in both rats and rabbits. Zanubrutinib was administered orally to pregnant rats during the period of organogenesis at doses of 30, 75, and 150 mg/kg/day. Malformations in the heart (2 or 3-chambered hearts) were noted at all dose levels in the absence of maternal toxicity. The dose of 30 mg/kg/day is approximately 5 times the exposure (AUC) in patients receiving the recommended dose of 160 mg twice daily.
Administration of zanubrutinib to pregnant rabbits during the period of organogenesis at 30, 70, and 150 mg/kg/day resulted in postimplantation loss at the highest dose. The dose of 150 mg/kg is approximately 32 times the exposure (AUC) in patients at the recommended dose and was associated with maternal toxicity.
In a pre and postnatal developmental toxicity study, zanubrutinib was administered orally to rats at doses of 30, 75, and 150 mg/kg/day from implantation through weaning. The offspring from the middle and high dose groups had decreased body weights preweaning, and all dose groups had adverse ocular findings (e.g., cataract, protruding eye). The dose of 30 mg/kg/day is approximately 5 times the AUC in patients receiving the recommended dose.
8.2 Lactation
Risk Summary
There are no data on the presence of zanubrutinib or its metabolites in human milk, the effects on the breastfed child, or the effects on milk production. Because of the potential for serious adverse reactions from BRUKINSA in a breastfed child, advise lactating women not to breastfeed during treatment with BRUKINSA and for two weeks following the last dose.
8.3 Females and Males of Reproductive Potential
BRUKINSA can cause embryo-fetal harm when administered to pregnant women [see Use in Specific Populations (8.1)].
Pregnancy Testing
Pregnancy testing is recommended for females of reproductive potential prior to initiating BRUKINSA therapy.
Contraception
Females
Advise female patients of reproductive potential to use effective contraception during treatment with BRUKINSA and for 1 week following the last dose of BRUKINSA. If this drug is used during pregnancy, or if the patient becomes pregnant while taking this drug, the patient should be informed of the potential hazard to a fetus.
Males
Advise men to avoid fathering a child while receiving BRUKINSA and for 1 week following the last dose of BRUKINSA.
8.4 Pediatric Use
Safety and effectiveness of BRUKINSA in pediatric patients have not been established.
8.5 Geriatric Use
Of the 1729 patients with MCL, MZL, WM, CLL/SLL, and FL in clinical studies with BRUKINSA, 59% were ≥65 years of age, and 21% were ≥75 years of age. Patients ≥65 years of age had numerically higher rates of Grade 3 or higher adverse reactions and serious adverse reactions (57% and 38%, respectively) than patients <65 years of age (51% and 29%, respectively). No overall differences in effectiveness were observed between younger and older patients.
8.6 Renal Impairment
No dosage modification is recommended in patients with mild, moderate, or severe renal impairment (CLcr ≥15 mL/min, estimated by Cockcroft-Gault). Monitor for BRUKINSA adverse reactions in patients on dialysis [see Clinical Pharmacology (12.3)].
8.7 Hepatic Impairment
Dosage modification of BRUKINSA is recommended in patients with severe hepatic impairment [see Dosage and Administration (2.2)]. The safety of BRUKINSA has not been evaluated in patients with severe hepatic impairment. No dosage modification is recommended in patients with mild to moderate hepatic impairment. Monitor for BRUKINSA adverse reactions in patients with hepatic impairment [see Clinical Pharmacology (12.3)].
Lactation: Advise not to breastfeed. (8.2)
DESCRIPTION SECTION
11 DESCRIPTION
BRUKINSA (zanubrutinib) is a kinase inhibitor. The empirical formula of zanubrutinib is C27H29N5O3and the chemical name is (S)-7-(1-acryloylpiperidin-4-yl)-2-(4-phenoxyphenyl)-4,5,6,7-tetrahydropyrazolo[1,5-a]pyrimidine-3-carboxamide. Zanubrutinib is a white to off-white powder, with a pH of 7.8 in saturated solution. The aqueous solubility of zanubrutinib is pH dependent, from very slightly soluble to practically insoluble.
The molecular weight of zanubrutinib is 471.55 Daltons.
Zanubrutinib has the following structure:
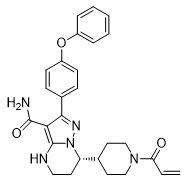
Each BRUKINSA capsule for oral administration contains 80 mg zanubrutinib and the following inactive ingredients: colloidal silicon dioxide, croscarmellose sodium, magnesium stearate, microcrystalline cellulose, and sodium lauryl sulfate. The capsule shell contains edible black ink, gelatin, and titanium dioxide.
CLINICAL PHARMACOLOGY SECTION
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
Zanubrutinib is a small-molecule inhibitor of Bruton's tyrosine kinase (BTK). Zanubrutinib forms a covalent bond with a cysteine residue in the BTK active site, leading to inhibition of BTK activity. BTK is a signaling molecule of the B-cell antigen receptor (BCR) and cytokine receptor pathways. In B-cells, BTK signaling results in activation of pathways necessary for B-cell proliferation, trafficking, chemotaxis, and adhesion. In nonclinical studies, zanubrutinib inhibited malignant B-cell proliferation and reduced tumor growth.
12.2 Pharmacodynamics
BTK Occupancy in PBMCs and Lymph Nodes
The median steady-state BTK occupancy in peripheral blood mononuclear cells was maintained at 100% over 24 hours at a total daily dose of 320 mg in patients with B-cell malignancies. The median steady-state BTK occupancy in lymph nodes was 94% to 100% following the approved recommended dosage.
Cardiac Electrophysiology
At the approved recommended doses (160 mg twice daily or 320 mg once daily), there were no clinically relevant effects on the QTc interval. The effect of BRUKINSA on the QTc interval above the therapeutic exposure has not been evaluated.
12.3 Pharmacokinetics
Zanubrutinib maximum plasma concentration (Cmax) and area under the plasma drug concentration over time curve (AUC) increase proportionally over a dosage range from 40 mg to 320 mg (0.13 to 1 time the recommended total daily dose). Limited systemic accumulation of zanubrutinib was observed following repeated administration.
The geometric mean (%CV) zanubrutinib steady-state daily AUC is 2,099 (42%) ng∙h/mL following 160 mg twice daily and 1,917 (59%) ng∙h/mL following 320 mg once daily. The geometric mean (%CV) zanubrutinib steady-state Cmax is 295 (55%) ng/mL following 160 mg twice daily and 537 (55%) ng/mL following 320 mg once daily.
Absorption
The median tmax of zanubrutinib is 2 hours.
Effect of Food
No clinically significant differences in zanubrutinib AUC or Cmax were observed following administration of a high-fat meal (approximately 1,000 calories with 50% of total caloric content from fat) in healthy subjects.
Distribution
The geometric mean (%CV) apparent volume of distribution (Vz/F) of zanubrutinib is 537 (73%) L. The plasma protein binding of zanubrutinib is approximately 94% and the blood-to-plasma ratio is 0.7 to 0.8.
Elimination
The mean half-life (t½) of zanubrutinib is approximately 2 to 4 hours following a single oral zanubrutinib dose of 160 mg or 320 mg. The geometric mean (%CV) apparent oral clearance (CL/F) of zanubrutinib is 128 (58%) L/h.
Metabolism
Zanubrutinib is primarily metabolized by cytochrome P450(CYP)3A.
Excretion
Following a single radiolabeled zanubrutinib dose of 320 mg to healthy subjects, approximately 87% of the dose was recovered in feces (38% unchanged) and 8% in urine (less than 1% unchanged).
Specific Populations
No clinically significant differences in the pharmacokinetics of zanubrutinib were observed based on age (19 to 90 years), sex, race (Asian, White, and Other), body weight (36 to 144 kg), or mild, moderate or severe renal impairment (CLcr ≥15 mL/min as estimated by Cockcroft-Gault). The effect of dialysis on zanubrutinib pharmacokinetics is unknown.
Hepatic Impairment
The total AUC of zanubrutinib increased by 11% in subjects with mild hepatic impairment (Child-Pugh class A), by 21% in subjects with moderate hepatic impairment (Child-Pugh class B), and by 60% in subjects with severe hepatic impairment (Child-Pugh class C) relative to subjects with normal liver function. The unbound AUC of zanubrutinib increased by 23% in subjects with mild hepatic impairment (Child-Pugh class A), by 43% in subjects with moderate hepatic impairment (Child-Pugh class B) and by 194% in subjects with severe hepatic impairment (Child-Pugh class C) relative to subjects with normal liver function.
Drug Interaction Studies
Clinical Studies and Model-Informed Approaches
CYP3A Inhibitors: Coadministration of multiple doses of CYP3A inhibitors increases zanubrutinib Cmax and AUC (Table 18).
Table 18: Observed or Predicted Increase in Zanubrutinib Exposure After Coadministration of CYP3A Inhibitors|
Coadministered CYP3A Inhibitor |
Increase in Zanubrutinib Cmax |
Increase in Zanubrutinib AUC |
|---|---|---|
| ||
|
Observed | ||
|
Itraconazole (200 mg once daily)* |
157% |
278% |
|
Fluconazole (400 mg once daily)† |
81% |
88% |
|
Diltiazem (180 mg once daily)† |
62% |
62% |
|
Voriconazole (200 mg twice daily)† |
229% |
230% |
|
Clarithromycin (250 mg twice daily)† |
101% |
92% |
|
Predicted | ||
|
Posaconazole suspension (100 mg once daily)‡ |
169% |
180% |
|
Posaconazole suspension (100 mg twice daily)‡ |
207% |
279% |
|
Posaconazole delayed-release tablets (300 mg once daily)‡ |
232% |
407% |
|
Posaconazole intravenously (300 mg once daily)‡ |
205% |
333% |
|
Itraconazole (200 mg once daily)‡ |
273% |
320% |
CYP3A Inducers: Coadministration of multiple doses of rifampin (strong CYP3A inducer) decreased the zanubrutinib Cmax by 92% and AUC by 93%. Coadministration of multiple doses of rifabutin (moderate CYP3A inducer) decreased the zanubrutinib Cmax by 48% and AUC by 44%.
Coadministration of multiple doses of efavirenz (moderate CYP3A inducer) is predicted to decrease zanubrutinib Cmax by 58% and AUC by 60%.
CYP3A Substrates: Coadministration of multiple doses of zanubrutinib decreased midazolam (CYP3A substrate) Cmax by 30% and AUC by 47%.
CYP2C19 Substrates: Coadministration of multiple doses of zanubrutinib decreased omeprazole (CYP2C19 substrate) Cmax by 20% and AUC by 36%.
Other CYP Substrates: No clinically significant differences were observed with warfarin (CYP2C9 substrate) pharmacokinetics when coadministered with zanubrutinib.
Transporter Systems: Coadministration of multiple doses of zanubrutinib increased digoxin (P-gp substrate) Cmax by 34% and AUC by 11%. No clinically significant differences in the pharmacokinetics of rosuvastatin (BCRP substrate) were observed when coadministered with zanubrutinib.
Gastric Acid Reducing Agents: No clinically significant differences in zanubrutinib pharmacokinetics were observed when coadministered with gastric acid reducing agents (proton pump inhibitors, H2-receptor antagonists).
In Vitro Studies
CYP Enzymes: Zanubrutinib is an inducer of CYP2B6 and CYP2C8.
Transporter Systems: Zanubrutinib is likely to be a substrate of P-gp. Zanubrutinib is not a substrate or inhibitor of OAT1, OAT3, OCT2, OATP1B1, or OATP1B3.
CLINICAL STUDIES SECTION
14 CLINICAL STUDIES
14.1 Mantle Cell Lymphoma
The efficacy of BRUKINSA was assessed in BGB-3111-206 [NCT03206970], a Phase 2, open-label, multicenter, single-arm trial of 86 previously treated patients with MCL who had received at least one prior therapy. BRUKINSA was given orally at a dose of 160 mg twice daily until disease progression or unacceptable toxicity.
The median age of patients was 60.5 years (range: 34 to 75) and the majority were male (78%). The median time since diagnosis to study entry was 30 months (range: 3 to 102) and the median number of prior therapies was 2 (range: 1 to 4). The most common prior regimens were CHOP-based (91%) followed by rituximab-based (74%). The majority of patients had extranodal involvement (71%) and refractory disease (52%). Blastoid variant of MCL was present in 14% of patients. The MIPI score was low in 58%, intermediate in 29%, and high risk in 13%.
The efficacy of BRUKINSA was also assessed in BGB-3111-AU-003 [NCT02343120], a Phase 1/2, open-label, dose-escalation, global, multicenter, single-arm trial of B cell malignancies including 32 previously treated MCL patients treated with BRUKINSA. BRUKINSA was given orally at doses of 160 mg twice daily or 320 mg daily. The median age of patients with previously treated MCL was 70 years (range: 42 to 86) and 38% of patients were ≥75 years old. Most patients were male (69%) and White (78%). The MIPI score was low in 28%, intermediate in 41%, and high risk in 31%.
Tumor response was according to the 2014 Lugano Classification for both studies, and the primary efficacy endpoint was overall response rate as assessed by an Independent Review Committee (IRC).
Table 19: Efficacy Results per IRC in Patients with MCL|
Study BGB-3111-206 |
Study BGB-3111-AU-003 | |
|---|---|---|
|
ORR: overall response rate, CR: complete response, PR: partial response, DOR: duration of response, CI: confidence interval, NE: not estimable. | ||
| ||
|
ORR (95% CI) |
84% (74, 91) |
84% (67, 95) |
|
CR |
59% |
22%* |
|
PR |
24% |
62% |
|
Median DOR in months (95% CI) |
19.5 (16.6, NE) |
18.5 (12.6, NE) |
14.2 Waldenström's Macroglobulinemia
The efficacy of BRUKINSA was evaluated in ASPEN [NCT03053440], a randomized, active control, open-label trial, comparing BRUKINSA and ibrutinib in patients with MYD88 L265P mutation (MYD88MUT) WM. Patients in Cohort 1 (n=201) were randomized 1:1 to receive BRUKINSA 160 mg twice daily or ibrutinib 420 mg once daily until disease progression or unacceptable toxicity. Randomization was stratified by number of prior therapies (0 vs 1-3 vs >3) and CXCR4 status (presence or absence of a WHIM-like mutation as measured by Sanger assay).
The major efficacy outcome was the response rate defined as PR or better as assessed by IRC based on standard consensus response criteria from the International Workshop on Waldenström's Macroglobulinemia (IWWM)-6 criteria. An additional efficacy outcome measure was duration of response (DOR).
The median age was 70 years (range: 38 to 90) and 68% were male. Of those enrolled, 2% were Asian, 91% were White, and 7% were of unknown race. ECOG performance status of 0 or 1 was present in 93% patients at baseline and 7% had a baseline ECOG performance status of 2. A total of 82% had relapsed/refractory disease with 85% having received prior alkylating agents and 91% prior anti-CD20 therapy. The median number of prior therapies in those with relapsed/refractory disease was 1 (range: 1 to 8). A total of 91 (45%) patients had International Prognostic Scoring System (IPSS) high WM.
The study did not meet statistical significance for the prespecified efficacy outcome of superior CR+VGPR as assessed by IRC, tested first in patients with R/R disease in ASPEN.
Table 20 shows the response rates in ASPEN based on IRC assessment.
Table 20: Response Rate and Duration of Response Based on IRC Assessment in ASPEN|
Standard IWWM-6* |
Modified IWWM-6† | |||
|---|---|---|---|---|
|
Response Category |
BRUKINSA |
Ibrutinib |
BRUKINSA |
Ibrutinib |
| ||||
|
Response rate (CR+VGPR+PR), n (%) |
79 (77.5) |
77 (77.8) |
79 (77.5) |
77 (77.8) |
|
95% CI (%)‡ |
(68.1, 85.1) |
(68.3, 85.5) |
(68.1, 85.1) |
(68.3, 85.5) |
|
Complete Response (CR) |
0 (0) |
0 (0) |
0 (0) |
0 (0) |
|
Very Good Partial Response (VGPR) |
16 (15.7) |
7 (7.1) |
29 (28.4) |
19 (19.2) |
|
Partial Response (PR) |
63 (61.8) |
70 (70.7) |
50 (49) |
58 (58.6) |
|
Duration of response (DOR), Event-free at 12 months (95% CI)§ |
94.4% |
87.9% |
94.4% |
87.9% |
ASPEN Cohort 2
Cohort 2 enrolled patients with MYD88 wildtype (MYD88WT) or MYD88 mutation unknown WM (N=26 and 2, respectively) and received BRUKINSA 160 mg twice daily. The median age was 72 years (range: 39 to 87) with 43% >75 years, 50% were male, 96% were White, and 4% were not reported (unknown race). Eighty-six percent of patients had a baseline ECOG performance status 0 or 1 and 14% had a baseline performance status of 2. Twenty-three of the 28 patients in Cohort 2 had relapsed or refractory disease.
In Cohort 2, response (CR+VGPR+PR) as assessed by IRC using IWWM-6 or modified IWWM-6 was seen in 50% (13 out of 26 response evaluable patients; 95% CI: 29.9, 70.1).
14.3 Marginal Zone Lymphoma
The efficacy of BRUKINSA was assessed in Study BGB-3111-214 [NCT03846427], an open-label, multicenter, single-arm trial that evaluated 66 patients with MZL who received at least one prior anti–CD20-based therapy. BRUKINSA was given orally at a dosage of 160 mg twice daily until disease progression or unacceptable toxicity. The median age was 70 years (range: 37 to 85); 55% were male; 38% had extranodal MZL, 38% nodal, 18% splenic, and 6% had unknown subtype. The median number of prior systemic therapies was 2 (range: 1 to 6), with 27% having 3 or more lines of systemic therapy; 88% had prior rituximab- based chemotherapy; 32% had refractory disease at study entry.
The efficacy of BRUKINSA was also assessed in BGB-3111-AU-003 [NCT02343120], an open-label, multicenter, single-arm trial that included 20 patients with previously treated MZL (45% having extranodal MZL, 25% nodal, 30% splenic). BRUKINSA was given orally at dosages of 160 mg twice daily or 320 mg once daily. The median age was 70 years (range: 52 to 85); 50% were male. The median number of prior systemic therapies was 2 (range: 1 to 5), with 20% having 3 or more lines of systemic therapy; 95% had prior rituximab-based chemotherapy.
Efficacy was based on overall response rate (ORR) and duration of response as assessed by an Independent Review Committee (IRC) using 2014 Lugano criteria (Table 21).
Table 21: Efficacy Results per IRC in Patients with MZL|
Parameter |
Study BGB-3111-214 |
Study BGB-3111-AU-003 |
|---|---|---|
|
ORR: overall response rate, CR: complete response, PR: partial response, DOR: duration of response, CI: confidence interval, NE: not estimable. | ||
| ||
|
Overall Response Rate (CT-based)***** | ||
|
ORR, n |
37 (56%) |
16 (80%) |
|
(95% CI, %) |
(43, 68) |
(56, 94) |
|
CR, n |
13 (20%) |
4 (20%) |
|
PR, n |
24 (36%) |
12 (60%) |
|
Time to Response | ||
|
Median (range), months |
2.9 (1.8, 11.1) |
2.9 (2.6, 23.1) |
|
Duration of Response**†** | ||
|
Median DOR (95% CI), months |
NE (NE, NE) |
NE (8.4, NE) |
|
Rate at 12 months (95% CI) |
85% (67, 93) |
72% (40, 88) |
In study BGB-3111-214, ORR prioritizing PET-CT when available (55 patients, with the remainder assessed by CT scan) was 67% (95% CI: 54, 78) with a CR rate of 26%.
14.4 Chronic Lymphocytic Leukemia or Small Lymphocytic Lymphoma
The efficacy of BRUKINSA in patients with CLL/SLL was evaluated in two randomized controlled trials.
SEQUOIA
The efficacy of BRUKINSA in patients with previously untreated CLL/SLL was evaluated in a multicenter, open-label trial (SEQUOIA; NCT03336333). The trial required patients to be unsuitable for FCR therapy defined as either age ≥65 years or age 18 to <65 with a total Cumulative Illness Rating Scale (CIRS) >6, creatinine clearance 30 to 69 mL/min, or history of serious or recurrent infection. Patients without 17p deletion (17p del) were randomized to receive either BRUKINSA 160 mg twice daily until disease progression or unacceptable toxicity (n=241) or bendamustine plus rituximab (BR) for 6 cycles (n=238). Bendamustine was dosed at 90 mg/m2/day intravenously on the first 2 days of each cycle, and rituximab was dosed at 375 mg/m2 on day 1 of Cycle 1 and 500 mg/m2 on day 1 of Cycles 2 to 6 with a 28-day cycle length. Randomization was stratified by age, Binet stage, immunoglobulin variable region heavy chain (IGHV) mutational status, and geographic region.
Additionally, the same BRUKINSA regimen was evaluated in 110 patients with previously untreated 17p del CLL/SLL in a non-randomized cohort.
Efficacy is summarized according to cohort.
Randomized Cohort: Previously Untreated CLL/SLL without 17p Deletion
In the randomized cohort of patients with previously untreated CLL/SLL without 17p deletion, the median age was 70 years; 62% were male, 89% were White, 3% were Asian, and 1% were Black. Fifty-three percent of patients had an unmutated IGHV gene and 29% had Binet Stage C disease. Baseline characteristics were generally similar between treatment arms.
Efficacy in this cohort was based on progression-free survival as assessed by an IRC. Efficacy results are presented in Table 22 and Figure 1.
Table 22: Efficacy Results per IRC in Patients with Previously Untreated CLL/SLL without 17p Deletion in SEQUOIA (Randomized Cohort)|
Parameter* |
CLL/SLL without del(17p) | |
|---|---|---|
|
BRUKINSA |
Bendamustine + Rituximab | |
|
CI=Confidence interval, CR=complete response, CRi=complete response with incomplete hematopoietic recovery, HR=hazard ratio, NE=not estimable, nPR=nodular partial response, ORR=overall response rate, PFS=progression-free survival, PR=partial response. | ||
| ||
|
Progression-free survival | ||
|
Number of Events, n |
36 (15%) |
71 (30%) |
|
Disease Progression |
27 (11%) |
59 (25%) |
|
Death |
9 (3.7%) |
12 (5%) |
|
Median PFS (95% CI), months† |
NE (NE, NE) |
33.7 (28.1, NE) |
|
HR (95% CI)‡ |
0.42 (0.28, 0.63) | |
|
P-value§ |
<0.0001 | |
|
Overall response rate**¶** | ||
|
ORR, n (%) |
225 (93) |
203 (85) |
|
95% CI, % |
(89, 96) |
(80, 90) |
|
CR, n (%) |
16 (7) |
36 (15) |
|
nPR, n (%) |
3 (1.2) |
14 (6) |
|
PR, n (%) |
206 (85) |
153 (64) |
Figure 1: Kaplan-Meier Plot of IRC-Assessed Progression-Free Survival in Patients with Previously Untreated CLL/SLL without 17p Deletion in SEQUOIA
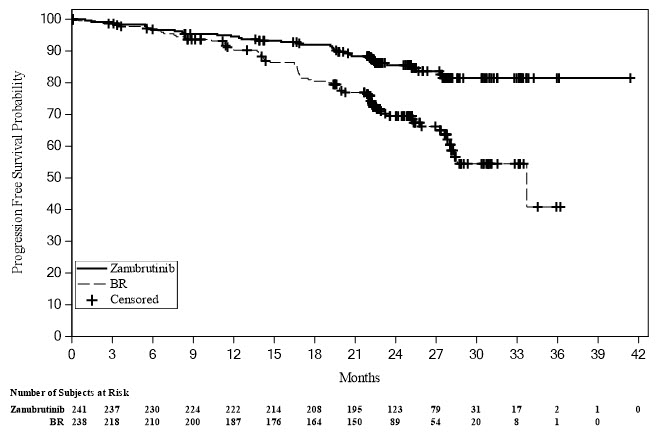
At the time of analysis, overall survival data were immature. With an estimated median follow-up of 25.7 months, median overall survival was not reached in either arm, with fewer than 7% of patients experiencing an event.
Single-Arm Cohort: Previously Untreated CLL/SLL with 17p Deletion
In this cohort, 110 patients with previously untreated CLL/SLL and centrally confirmed 17p deletion received BRUKINSA 160 mg twice daily until disease progression or unacceptable toxicity.
The median age was 70, 71% were male, 95% were White, and 1% were Asian. Sixty percent of patients had an unmutated IGHV gene and 35% had Binet Stage C disease.
Efficacy was based on overall response rate and duration of response as assessed by an IRC. Efficacy results are presented in Table 23.
Table 23: Efficacy Results per IRC in Patients with Previously Untreated CLL/SLL and 17p Deletion in SEQUOIA|
Parameter* |
del(17p) CLL/SLL |
|---|---|
|
DOR=duration of response. A + sign indicates a censored observation. | |
| |
|
Overall response rate**†** | |
|
ORR, n (%) |
97 (88) |
|
(95% CI, %) |
(81, 94) |
|
CR, n (%) |
7 (6) |
|
nPR, n (%) |
2 (1.8) |
|
PR, n (%) |
88 (80) |
|
Time to response | |
|
Median (range), months |
2.9 (1.9 to 13.9) |
|
Duration of response | |
|
Median DOR (95% CI),‡ months |
NE (NE, NE) |
|
Range, months |
(5.6 to 35.9+) |
|
Rate at 12 months, % (95% CI)‡ |
96 (89, 98) |
|
Rate at 18 months, % (95% CI)‡ |
95 (88, 98) |
ALPINE
The efficacy of BRUKINSA in patients with relapsed or refractory CLL/SLL was evaluated in ALPINE, a randomized, multicenter, open-label, actively controlled trial (NCT03734016). The trial enrolled 652 patients with relapsed or refractory CLL/SLL after at least 1 systemic therapy. The patients were randomized in a 1:1 ratio to receive either BRUKINSA 160 mg orally twice daily (n=327) or ibrutinib 420 mg orally once daily (n=325), each administered until disease progression or unacceptable toxicity.
Randomization was stratified by age, geographic region, refractoriness to last therapy, and 17p deletion/TP53mutation status.
Baseline characteristics were similar between treatment arms. Overall, the median age was 67 years, 68% were male, 81% were White, 14% were Asian, and 1% were Black. Forty-three percent had advanced stage disease, 73% had an unmutated IGHV gene, and 23% had 17p deletion orTP53 mutation. Patients had a median of one prior line of therapy (range: 1-8), 18% of patients had ≥3 prior lines of therapy, 78% had prior chemoimmunotherapy, and 2.3% had prior BCL2 inhibitor.
Efficacy was based on overall response rate and duration of response as determined by an IRC. For progression-free survival per IRC, the final analysis occurred with a median follow-up of 31 months. Efficacy results are shown in Table 24 and Figure 2.
Table 24: Efficacy Results per IRC in Patients with Relapsed or Refractory CLL/SLL in ALPINE|
Parameter* |
BRUKINSA |
Ibrutinib |
|---|---|---|
|
CI=Confidence interval, CR=complete response, CRi=complete response with incomplete hematopoietic recovery, DOR=duration of response, HR=hazard ratio, NE=not estimable, nPR=nodular partial response, ORR=overall response rate, PR=partial response. A + sign indicates a censored observation. | ||
Þ ß | ||
|
Overall response rate**†** | ||
|
ORR, n (%) |
263 (80) |
237 (73) |
|
(95% CI, %) |
(76, 85) |
(68, 78) |
|
CR, n (%) |
13 (4) |
8 (2.5) |
|
nPR, n (%) |
1 (0.3) |
0 (0) |
|
PR, n (%) |
249 (76) |
229 (70) |
|
Response Rate Ratio (95% CI)‡ |
1.10 (1.01, 1.20) | |
|
2-sided p-value§ |
0.0264 | |
|
Duration of response | ||
|
Median DOR (95% CI)¶ |
NE (NE, NE) |
NE (NE, NE) |
|
Range, months |
(1.4 to 30.4+) |
(1.9+ to 30.8+) |
|
Rate at 12 months, % (95% CI)¶ |
92 (87, 95) |
86 (80, 91) |
|
Progression-free survival | ||
|
Events, n (%) |
88 (27) |
120 (37) |
|
Median PFS (95% CI), months# |
NE (34.3, NE) |
35 (33.2, 44.3) |
|
HR (95% CI)Þ |
0.65 (0.49, 0.86) | |
|
2-sided p-valueß |
0.0024 |
The median time to response was 5.5 months for BRUKINSA and 5.6 months for ibrutinib.
Figure 2: Kaplan-Meier Plot of Progression-Free Survival by IRC in ALPINE
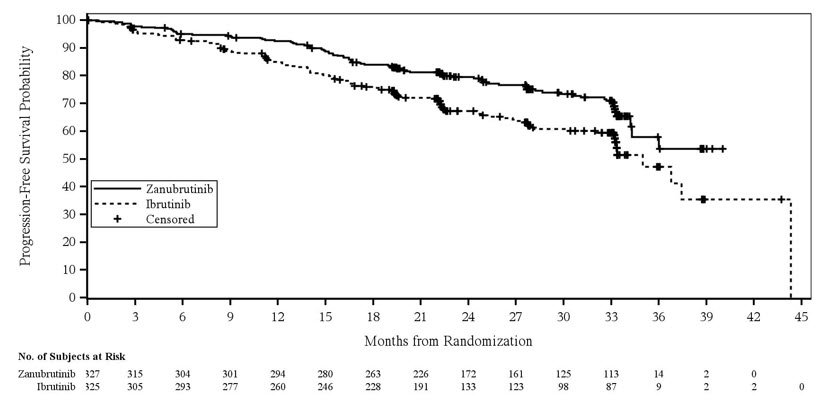
At the time of final analysis, the median overall survival was not reached in either arm. There were a total of 108 deaths: 48 (14.7%) in the zanubrutinib arm and 60 (18.5%) in the ibrutinib arm.
14.5 Follicular Lymphoma
The efficacy of BRUKINSA, in combination with obinutuzumab, was evaluated in Study BGB-3111-212 (ROSEWOOD; NCT03332017), an open-label, multicenter, randomized trial that enrolled 217 adult patients with relapsed or refractory FL after at least 2 prior systemic treatments. The study required prior receipt of an anti-CD20 antibody and an alkylator-based combination therapy, and excluded patients with FL Grade 3b, transformed lymphoma, and prior exposure to a BTK inhibitor.
Patients were randomized in a 2:1 ratio to receive either BRUKINSA 160 mg orally twice daily until disease progression or unacceptable toxicity plus obinutuzumab, or obinutuzumab alone. Obinutuzumab was administered 1,000 mg intravenously on days 1, 8, and 15 of Cycle 1, 1,000 mg on Day 1 of Cycles 2 to 6; and then 1,000 mg every 8 weeks for up to 20 doses. At the discretion of the investigator, obinutuzumab could be administered as 100 mg on Day 1 and 900 mg on Day 2 of Cycle 1.
Randomization was stratified by the number of prior lines of therapy (2 to 3 vs ˃3), rituximab-refractory status (yes vs no), and geographic region.
Of the 217 patients randomized (145 to BRUKINSA plus obinutuzumab, 72 to obinutuzumab monotherapy), the median age was 64 years (range: 31 to 88), 50% were male, 64% were White, and 22% were Asian. In total, 83% had stage 3 or 4 disease and 57% met Groupe d'Etude des Lymphomes Folliculaires (GELF) criteria at enrollment. Patients had a median of 3 prior lines of therapy (range: 2-11), with 27% of patients having more than 3 prior lines of therapy.
In the BRUKINSA in combination with obinutuzumab arm, 5% had received lenalidomide plus rituximab, 21% had received stem cell transplantation, 53% had refractory disease to rituximab, and 37% had progression of disease within 24 months of the first systemic therapy.
Efficacy was based on overall response rate and duration of response, as determined by an IRC. Efficacy results are shown in Table 25. The median time to response in the BRUKINSA combination arm was 2.8 months (range 2 to 23 months).
Table 25: Efficacy Results per IRC in Patients with Relapsed or Refractory Follicular Lymphoma|
Parameter |
BRUKINSA + Obinutuzumab |
Obinutuzumab |
|---|---|---|
|
CI=Confidence interval, CR=complete response, DOR=duration of response, NE=not estimable, ORR=overall response rate, PR=partial response. | ||
| ||
|
Overall response rate | ||
|
ORR, n (%) |
100 (69) |
33 (46) |
|
(95% CI)* |
(61, 76) |
(34, 58) |
|
CR |
57 (39) |
14 (19) |
|
PR |
43 (30) |
19 (26) |
|
Risk difference, % (95% CI)† |
22.7 (9, 36.5) | |
|
2-sided p-value†,‡ |
0.0012 | |
|
Duration of response | ||
|
Median DOR (95% CI),§ months |
NE (25.3, NE) |
14 (9.2, 25.1) |
The estimated DOR rate at 18 months was 69% (95% CI: 58, 78) in the BRUKINSA combination arm and 42% (95% CI: 23, 60) in the obinutuzumab monotherapy arm.
SPL UNCLASSIFIED SECTION
Manufactured for:
BeiGene USA, Inc.
1840 Gateway Dr., FL 3
San Mateo, CA 94404
BRUKINSA® is a registered trademark owned by BeiGene, Ltd.
© BeiGene, Ltd. 2024
SPL PATIENT PACKAGE INSERT SECTION
|
PATIENT INFORMATION | |||
|---|---|---|---|
|
This Patient Information has been approved by the U.S. Food and Drug Administration |
Revised: 3/2024 | ||
|
What is BRUKINSA?
It is not known if BRUKINSA is safe and effective in children. | |||
|
Before taking BRUKINSA, tell your healthcare provider about all of your medical conditions, including if you:
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements. Taking BRUKINSA with certain other medications may affect how BRUKINSA works and can cause side effects. | |||
|
How should I take BRUKINSA?
| |||
|
What are the possible side effects of BRUKINSA? *Bleeding problems (hemorrhage). Bleeding problems are common with BRUKINSA, and can be serious and may lead to death. Your risk of bleeding may increase if you are also taking a blood thinner medicine. Tell your healthcare provider if you have any signs or symptoms of bleeding, including: | |||
|
| ||
|
Infections that can be serious and may lead to death. Tell your healthcare provider right away if you have fever, chills, or flu-like symptoms. Decrease in blood cell counts (white blood cells, platelets, and red blood cells). Your healthcare provider should do blood tests during treatment with BRUKINSA to check your blood counts. Second primary cancers. New cancers have happened in people during treatment with BRUKINSA, including cancers of the skin or other organs. Your healthcare provider will check you for other cancers during treatment with BRUKINSA. Use sun protection when you are outside in sunlight. Heart rhythm problems (atrial fibrillation, atrial flutter, and ventricular arrhythmias) that can be serious and may lead to death. Tell your healthcare provider if you have any of the following signs or symptoms: | |||
|
| ||
|
The most common side effects of BRUKINSA include: | |||
|
| ||
|
These are not all the possible side effects of BRUKINSA. | |||
|
How should I store BRUKINSA?
Keep BRUKINSA and all medicines out of the reach of children. | |||
|
General information about the safe and effective use of BRUKINSA. | |||
|
What are the ingredients in BRUKINSA? |
NONCLINICAL TOXICOLOGY SECTION
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenicity studies have not been conducted with zanubrutinib.
Zanubrutinib was not mutagenic in a bacterial mutagenicity (Ames) assay, was not clastogenic in a chromosome aberration assay in mammalian (CHO) cells, nor was it clastogenic in an in vivo bone marrow micronucleus assay in rats.
A combined male and female fertility and early embryonic development study was conducted in rats at oral zanubrutinib doses of 30 to 300 mg/kg/day. Male rats were dosed 4 weeks prior to mating and through mating and female rats were dosed 2 weeks prior to mating and to gestation day 7. No effect on male or female fertility was noted at lower doses, but at the highest dose tested, morphological abnormalities in sperm and increased postimplantation loss were noted. The high dose of 300 mg/kg/day is approximately 10 times the human recommended dose, based on body surface area.
HOW SUPPLIED SECTION
16 HOW SUPPLIED/STORAGE AND HANDLING
How Supplied
|
Package Size |
Content |
NDC Number |
|---|---|---|
|
120-count |
Bottle with a child-resistant cap containing 120 capsules |
72579-011-02 |
Storage
Store at 20°C to 25°C (68°F to 77°F); excursions permitted between 15°C to 30°C (59°F to 86°F) [See USP Controlled Room Temperature].
INFORMATION FOR PATIENTS SECTION
17 PATIENT COUNSELING INFORMATION
Advise patients to read the FDA-approved patient labeling (Patient Information).
Hemorrhage
Inform patients to report signs or symptoms of severe bleeding. Inform patients that BRUKINSA may need to be interrupted for major surgeries or procedures [see Warnings and Precautions (5.1)].
Infections
Inform patients to report signs or symptoms suggestive of infection [see Warnings and Precautions (5.2)].
Cytopenias
Inform patients that they will need periodic blood tests to check blood counts during treatment with BRUKINSA [see Warnings and Precautions (5.3)].
Second Primary Malignancies
Inform patients that other malignancies have been reported in patients who have been treated with BRUKINSA, including skin cancer and other solid tumors. Advise patients to use sun protection and have monitoring for development of other cancers [see Warnings and Precautions (5.4)].
Cardiac Arrhythmias
Counsel patients to report any signs of palpitations, lightheadedness, dizziness, fainting, shortness of breath, and chest discomfort [see Warnings and Precautions (5.5)].
Embryo-Fetal Toxicity
Advise pregnant women and females of reproductive potential of the potential hazard to a fetus and to use effective contraception during treatment and for 1 week after the last dose of BRUKINSA [see Warnings and Precautions (5.6)]. Advise males with female sexual partners of reproductive potential to use effective contraception during BRUKINSA treatment and for 1 week after the last dose of BRUKINSA [see Use in Specific Populations (8.3)].
Lactation
Advise females not to breastfeed during treatment with BRUKINSA and for 2 weeks after the last dose [see Use in Specific Populations (8.2)].
Administration Instructions
BRUKINSA may be taken with or without food. Advise patients that BRUKINSA capsules should be swallowed whole with a glass of water, without being opened, broken, or chewed [see Dosage and Administration (2.1)].
Missed Dose
Advise patients that if they miss a dose of BRUKINSA, they may still take it as soon as possible on the same day with a return to the normal schedule the following day [see Dosage and Administration (2.1)].
Drug Interactions
Advise patients to inform their healthcare providers of all concomitant medications, including over-the-counter medications, vitamins, and herbal products [see Drug Interactions (7.1)].
