Esmolol Hydrochloride
These highlights do not include all the information needed to use safely and effectively. See full prescribing information for . Initial U.S. Approval: 1986
94f069f9-dd52-4a69-a103-ebdb4294f088
HUMAN PRESCRIPTION DRUG LABEL
Sep 15, 2023
Mylan Institutional LLC
DUNS: 790384502
Products 1
Detailed information about drug products covered under this FDA approval, including NDC codes, dosage forms, ingredients, and administration routes.
esmolol hydrochloride
Product Details
FDA regulatory identification and product classification information
FDA Identifiers
Product Classification
Product Specifications
INGREDIENTS (6)
Drug Labeling Information
PACKAGE LABEL.PRINCIPAL DISPLAY PANEL
PRINCIPAL DISPLAY PANEL - 100 mg/10 mL
NDC 67457-182-10
Esmolol
Hydrochloride
Injection
100 mg/10 mL
(10 mg/mL)
For Intravenous Use
Rx only 10 x 10 mL Single-Dose Vials
Contains no preservatives.
Discard unused portion.
Each mL contains: 10 mg Esmolol Hydrochloride, USP and Water for
Injection. Buffered with 1.688 mg Sodium
Acetate Anhydrous (equivalent to 2.8 mg Sodium Acetate Trihydrate) and 0.546
mg Glacial Acetic Acid.
Sodium Hydroxide and/or Hydrochloric Acid added for pH adjustment. pH range is
4.5 to 5.5.
Usual Dosage: See accompanying prescribing information.
Store at 20° to 25°C (68° to 77°F). [See USP Controlled Room Temperature.]
Protect from freezing.
Avoid excessive heat.
Avoid contact with alkalies. Do not use if discolored or if a precipitate is present.
Manufactured for:
Mylan Institutional LLC
Morgantown, WV 26505 U.S.A.
Manufactured by:
Mylan Institutional
Galway, Ireland
MI:182:10C:R6
Mylan.com

INDICATIONS & USAGE SECTION
1 INDICATIONS AND USAGE
1.1 Supraventricular Tachycardia or Noncompensatory Sinus Tachycardia
Esmolol hydrochloride injection is indicated for the rapid control of ventricular rate in patients with atrial fibrillation or atrial flutter in perioperative, postoperative, or other emergent circumstances where short term control of ventricular rate with a short-acting agent is desirable. Esmolol hydrochloride injection is also indicated in noncompensatory sinus tachycardia where, in the physician’s judgment, the rapid heart rate requires specific intervention. Esmolol hydrochloride injection is intended for short-term use.
1.2 Intraoperative and Postoperative Tachycardia and/or Hypertension
Esmolol hydrochloride injection is indicated for the short-term treatment of tachycardia and hypertension that occur during induction and tracheal intubation, during surgery, on emergence from anesthesia and in the postoperative period, when in the physician’s judgment such specific intervention is considered indicated.
Use of esmolol hydrochloride injection to prevent such events is not recommended.
Esmolol hydrochloride injection is a beta adrenergic blocker indicated for the short-term treatment of:
•
Control of ventricular rate in supraventricular tachycardia including atrial fibrillation and atrial flutter and control of heart rate in noncompensatory sinus tachycardia (1.1)
•
Control of perioperative tachycardia and hypertension (1.2)
WARNINGS AND PRECAUTIONS SECTION
5 WARNINGS AND PRECAUTIONS
5.1 Hypotension
Hypotension can occur at any dose but is dose-related. Patients with hemodynamic compromise or on interacting medications are at particular risk. Severe reactions may include loss of consciousness, cardiac arrest, and death. For control of ventricular heart rate, maintenance doses greater than 200 mcg per kg per min are not recommended. Monitor patients closely, especially if pretreatment blood pressure is low. In case of an unacceptable drop in blood pressure, reduce or stop esmolol hydrochloride injection. Decrease of dose or termination of infusion reverses hypotension, usually within 30 minutes.
5.2 Bradycardia
Bradycardia, including sinus pause, heart block, severe bradycardia, and cardiac arrest have occurred with the use of esmolol hydrochloride injection. Patients with first-degree atrioventricular block, sinus node dysfunction, or conduction disorders may be at increased risk. Monitor heart rate and rhythm in patients receiving esmolol hydrochloride injection [see Contraindications (4)].
If severe bradycardia develops, reduce or stop esmolol hydrochloride injection.
5.3 Cardiac Failure
Beta blockers, like esmolol hydrochloride injection, can cause depression of myocardial contractility and may precipitate heart failure and cardiogenic shock. At the first sign or symptom of impending cardiac failure, stop esmolol hydrochloride injection and start supportive therapy [see Overdosage (10)].
5.4 Intraoperative and Postoperative Tachycardia and/or Hypertension
Monitor vital signs closely and titrate esmolol hydrochloride injection slowly in the treatment of patients whose blood pressure is primarily driven by vasoconstriction associated with hypothermia.
5.5 Reactive Airways Disease
Patients with reactive airways disease should, in general, not receive beta blockers. Because of its relative beta1 selectivity and titratability, titrate esmolol hydrochloride injection to the lowest possible effective dose. In the event of bronchospasm, stop the infusion immediately; a beta2 stimulating agent may be administered with appropriate monitoring of ventricular rates.
5.6 Hypoglycemia
Beta-blockers may prevent early warning signs of hypoglycemia, such as tachycardia, and increase the risk for severe or prolonged hypoglycemia at any time during treatment, especially in patients with diabetes mellitus or children and patients who are fasting (i.e., surgery, not eating regularly, or are vomiting). If severe hypoglycemia occurs, patients should be instructed to seek emergency treatment.
5.7 Infusion Site Reactions
Infusion site reactions have occurred with the use of esmolol hydrochloride injection. They include irritation, inflammation, and severe reactions (thrombophlebitis, necrosis, and blistering), in particular when associated with extravasation [see Adverse Reactions (6)]. Avoid infusions into small veins or through a butterfly catheter.
If a local infusion site reaction develops, use an alternative infusion site and avoid extravasation.
5.8 Use in Patients with Prinzmetal’s Angina
Beta blockers may exacerbate anginal attacks in patients with Prinzmetal’s angina because of unopposed alpha receptor–mediated coronary artery vasoconstriction. Do not use nonselective beta blockers.
5.9 Use in Patients with Pheochromocytoma
If esmolol hydrochloride injection is used in the setting of pheochromocytoma, give it in combination with an alpha-blocker, and only after the alpha-blocker has been initiated. Administration of beta-blockers alone in the setting of pheochromocytoma has been associated with a paradoxical increase in blood pressure from the attenuation of beta-mediated vasodilation in skeletal muscle.
5.10 Use in Hypovolemic Patients
In hypovolemic patients, esmolol hydrochloride injection can attenuate reflex tachycardia and increase the risk of hypotension.
5.11 Use in Patients with Peripheral Circulatory Disorders
In patients with peripheral circulatory disorders (including Raynaud’s disease or syndrome, and peripheral occlusive vascular disease), esmolol hydrochloride injection may aggravate peripheral circulatory disorders.
5.12 Abrupt Discontinuation of Esmolol Hydrochloride Injection
Severe exacerbations of angina, myocardial infarction, and ventricular arrhythmias have been reported in patients with coronary artery disease upon abrupt discontinuation of beta blocker therapy. Observe patients for signs of myocardial ischemia when discontinuing esmolol hydrochloride injection.
Heart rate increases moderately above pretreatment levels 30 minutes after esmolol hydrochloride injection discontinuation.
5.13 Hyperkalemia
Beta blockers, including esmolol hydrochloride injection, have been associated with increases in serum potassium levels and hyperkalemia. The risk is increased in patients with risk factors such as renal impairment. Intravenous administration of beta blockers has been reported to cause potentially life- threatening hyperkalemia in hemodialysis patients. Monitor serum electrolytes during therapy with esmolol hydrochloride injection.
5.14 Use in Patients with Metabolic Acidosis
Beta blockers, including esmolol hydrochloride injection, have been reported to cause hyperkalemic renal tubular acidosis. Acidosis in general may be associated with reduced cardiac contractility.
5.15 Use in Patients with Hyperthyroidism
Beta-adrenergic blockade may mask certain clinical signs (e.g., tachycardia) of hyperthyroidism. Abrupt withdrawal of beta blockade might precipitate a thyroid storm; therefore, monitor patients for signs of thyrotoxicosis when withdrawing beta blocking therapy.
5.16 Use in Patients at Risk of Severe Acute Hypersensitivity Reactions
When using beta blockers, patients at risk of anaphylactic reactions may be more reactive to allergen exposure (accidental, diagnostic, or therapeutic).
Patients using beta blockers may be unresponsive to the usual doses of epinephrine used to treat anaphylactic or anaphylactoid reactions [see Drug Interactions (7)].
•
Risk of hypotension, bradycardia, and cardiac failure: Monitor for signs and symptoms of cardiovascular adverse effects. Reduce or discontinue use (5.1, 5.2, 5.3, 5.10)
•
Risk of exacerbating reactive airway disease (5.5)
•
Diabetes: May mask symptoms of hypoglycemia and alter glucose levels; monitor (5.6)
•
Risk of unopposed alpha-agonism and severe hypertension in untreated pheochromocytoma (5.9)
•
Risk of myocardial ischemia when abruptly discontinued in patients with coronary artery disease (5.12, 5.15)
ADVERSE REACTIONS SECTION
6 ADVERSE REACTIONS
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
The following adverse reaction rates are based on use of esmolol hydrochloride injection in clinical trials involving 369 patients with supraventricular tachycardia and over 600 intraoperative and postoperative patients enrolled in clinical trials. Most adverse effects observed in controlled clinical trial settings have been mild and transient. The most important and common adverse effect has been hypotension [see Warnings and Precautions (5.1)]. Deaths have been reported in post-marketing experience occurring during complex clinical states where esmolol hydrochloride injection was presumably being used simply to control ventricular rate [see Warnings and Precautions (5.5)].
Table 3: Clinical Trial Adverse Reactions (Frequency ≥ 3%)
| ||
|
System Organ Class (SOC) |
Preferred MedDRA Term |
Frequency |
|
VASCULAR DISORDERS |
Hypotension* Asymptomatic hypotension Symptomatic hypotension (hyperhidrosis, dizziness) |
25% 12% |
|
GENERAL DISORDERS AND ADMINISTRATION SITE CONDITIONS |
Infusion site reactions (inflammation and induration) |
8% |
|
GASTROINTESTINAL DISORDERS |
Nausea |
7% |
|
NERVOUS SYSTEM DISORDERS |
Dizziness |
3% |
|
Somnolence |
3% |
Clinical Trial Adverse Reactions (Frequency < 3%):
Psychiatric Disorders:
Confusional state and agitation (~2%)
Anxiety, depression and abnormal thinking (< 1%)
Nervous System Disorders:
Headache (~2%)
Paresthesia, syncope, speech disorder, and lightheadedness (< 1%)
Convulsions (< 1%), with one death
Vascular Disorders:
Peripheral ischemia (~1%)
Pallor and flushing (< 1%)
Gastrointestinal Disorders:
Vomiting (~1%)
Dyspepsia, constipation, dry mouth, and abdominal discomfort (< 1%)
Renal and Urinary Disorders:
Urinary retention (< 1%)
6.2 Post-Marketing Experience
In addition to the adverse reactions reported in clinical trials, the following adverse reactions have been reported in the post-marketing experience. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to estimate reliably their frequency or to establish a causal relationship to drug exposure.
Cardiac Disorders:
Cardiac arrest, Coronary arteriospasm
Skin and Subcutaneous Tissue Disorders:
Angioedema, Urticaria, Psoriasis
Most common adverse reactions (incidence > 10%) are symptomatic hypotension (hyperhidrosis, dizziness) and asymptomatic hypotension (6)
**To report SUSPECTED ADVERSE REACTIONS, contactMylan at 1-877-446-3679 (1-877-4-INFO-RX) or FDA at 1-800-FDA-1088 or **www.fda.gov/medwatch.
DOSAGE & ADMINISTRATION SECTION
2 DOSAGE AND ADMINISTRATION
2.1 Dosing for the Treatment of Supraventricular Tachycardia or
Noncompensatory Sinus Tachycardia
Esmolol hydrochloride injection is administered by continuous intravenous infusion with or without a loading dose. Additional loading doses and/or titration of the maintenance infusion (step-wise dosing) may be necessary based on desired ventricular response.
Table 1: Step-Wise Dosing|
Step |
Action |
|
1 |
Optional loading dose (500 mcg per kg over 1 minute), then 50 mcg per kg per min for 4 min |
|
2 |
Optional loading dose if necessary, then 100 mcg per kg per min for 4 min |
|
3 |
Optional loading dose if necessary, then 150 mcg per kg per min for 4 min |
|
4 |
If necessary, increase dose to 200 mcg per kg per min |
In the absence of loading doses, continuous infusion of a single concentration of esmolol reaches pharmacokinetic and pharmacodynamic steady-state in about 30 minutes.
The effective maintenance dose for continuous and step-wise dosing is 50 to 200 mcg per kg per minute, although doses as low as 25 mcg per kg per minute have been adequate. Dosages greater than 200 mcg per kg per minute provide little added heart rate lowering effect, and the rate of adverse reactions increases.
Maintenance infusions may be continued for up to 48 hours.
2.2 Intraoperative and Postoperative Tachycardia and Hypertension
In this setting it is not always advisable to slowly titrate to a therapeutic effect. Therefore two dosing options are presented: immediate control and gradual control.
Immediate Control
•
Administer 1 mg per kg as a bolus dose over 30 seconds followed by an infusion of 150 mcg per kg per min if necessary.
•
Adjust the infusion rate as required to maintain desired heart rate and blood pressure. Refer to Maximum Recommended Doses below.
Gradual Control
•
Administer 500 mcg per kg as a bolus dose over 1 minute followed by a maintenance infusion of 50 mcg per kg per min for 4 minutes.
•
Depending on the response obtained, continue dosing as outlined for supraventricular tachycardia. Refer to Maximum Recommended Doses below.
Maximum Recommended Doses
•
For the treatment of tachycardia, maintenance infusion dosages greater than 200 mcg per kg per min are not recommended; dosages greater than 200 mcg per kg per min provide little additional heart rate-lowering effect, and the rate of adverse reactions increases.
•
For the treatment of hypertension, higher maintenance infusion dosages (250-300 mcg per kg per min) may be required. The safety of doses above 300 mcg per kg per minute has not been studied.
2.3 Transition from Esmolol Hydrochloride Injection Therapy to Alternative
Drugs
After patients achieve adequate control of the heart rate and a stable clinical status, transition to alternative antiarrhythmic drugs may be accomplished.
When transitioning from esmolol hydrochloride injection to alternative drugs, the physician should carefully consider the labeling instructions of the alternative drug selected and reduce the dosage of esmolol hydrochloride injection as follows:
Thirty minutes following the first dose of the alternative drug, reduce the esmolol hydrochloride infusion rate by one-half (50%).
After administration of the second dose of the alternative drug, monitor the patient's response and if satisfactory control is maintained for the first hour, discontinue the esmolol hydrochloride infusion.
2.4 Directions for Use
Esmolol hydrochloride injection is available in a single-dose vial. Esmolol hydrochloride injection is not compatible with Sodium Bicarbonate (5%) solution (limited stability) or furosemide (precipitation).
Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit.
Discard unused portion.
Single-Dose Vial
The single-dose vial may be used to administer a loading dosage by hand-held syringe while the maintenance infusion is being prepared.
•
Administer intravenously (2.1, 2.2)
•
Titrate using ventricular rate or blood pressure at ≥ 4-minute intervals. (2.1, 2.2)
•
Supraventricular tachycardia (SVT) or noncompensatory sinus tachycardia (2.1)
•
Optional loading dose: 500 mcg per kg infused over one minute
•
Then 50 mcg per kg per minute for the next 4 minutes
•
Adjust dose as needed to a maximum of 200 mcg per kg per minute.
•
Additional loading doses may be administered
•
Perioperative tachycardia and hypertension (2.2)
•
Loading dose: 500 mcg per kg over 1 minute for gradual control (1 mg per kg over 30 seconds for immediate control)
•
Then 50 mcg per kg per min for gradual control (150 mcg per kg per minute for immediate control) adjusted to a maximum of 200 (tachycardia) or 300 (hypertension) mcg per kg per min (2.2)
DOSAGE FORMS & STRENGTHS SECTION
3 DOSAGE FORMS AND STRENGTHS
Table 2: Esmolol Hydrochloride Injection Presentation|
Product Name |
Esmolol Hydrochloride Injection |
|
Total Dose |
100 mg/10 mL |
|
Esmolol Hydrochloride Concentration |
10 mg/mL |
|
Packaging |
10 mL Single-Dose Vial |
Injection: 100 mg/10 mL (10 mg/mL) in 10 mL single-dose vial (3)
USE IN SPECIFIC POPULATIONS SECTION
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Esmolol hydrochloride has been shown to produce increased fetal resorptions with minimal maternal toxicity in rabbits when given in doses approximately 8 times the maximum human maintenance dose (300 mcg/kg/min). There are no adequate and well-controlled studies in pregnant women. Esmolol hydrochloride injection should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
Teratogenicity studies in rats at intravenous dosages of esmolol hydrochloride up to 3000 mcg/kg/min (10 times the maximum human maintenance dosage) for 30 minutes daily produced no evidence of maternal toxicity, embryotoxicity or teratogenicity, while a dosage of 10,000 mcg/kg/min produced maternal toxicity and lethality. In rabbits, intravenous dosages up to 1000 mcg/kg/min for 30 minutes daily produced no evidence of maternal toxicity, embryotoxicity or teratogenicity, while 2500 mcg/kg/min produced minimal maternal toxicity and increased fetal resorptions.
8.2 Labor and Delivery
Although there are no adequate and well-controlled studies in pregnant women, use of esmolol in the last trimester of pregnancy or during labor or delivery has been reported to cause fetal bradycardia, which continued after termination of drug infusion. Esmolol hydrochloride injection should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
8.3 Nursing Mothers
It is not known whether this drug is excreted in human milk. Because many drugs are excreted in human milk and because of the potential for serious adverse reactions in nursing infants from esmolol hydrochloride injection, a decision should be made whether to discontinue nursing or to discontinue the drug, taking into account the importance of the drug to the mother.
8.4 Pediatric Use
The safety and effectiveness of esmolol hydrochloride injection in pediatric patients have not been established.
8.5 Geriatric Use
Clinical studies of esmolol hydrochloride injection did not include sufficient numbers of subjects aged 65 and over to determine whether they responded differently from younger subjects. Other reported clinical experience has not identified differences in responses between the elderly and younger patients. In general, dose selection for an elderly patient should usually start at the low end of the dosing range, reflecting greater frequency of decreased renal or cardiac function and of concomitant disease or other drug therapy.
8.6 Hepatic Impairment
No special precautions are necessary in patients with hepatic impairment because esmolol hydrochloride injection is metabolized by red-blood cell esterases [see Clinical Pharmacology (12)].
8.7 Renal Impairment
No dosage adjustment is required for esmolol in patients with renal impairment receiving a maintenance infusion of esmolol 150 mcg/kg for 4 hours. There is no information on the tolerability of maintenance infusions of esmolol using rates in excess of 150 mcg/kg or maintained longer than 4 hours [see Clinical Pharmacology (12)].
OVERDOSAGE SECTION
10 OVERDOSAGE
10.1 Signs and Symptoms of Overdose
Overdoses of esmolol hydrochloride injection can cause cardiac and central nervous system effects. These effects may precipitate severe signs, symptoms, sequelae, and complications (for example, severe cardiac and respiratory failure, including shock and coma), and may be fatal. Continuous monitoring of the patient is required.
•
Cardiac effects include bradycardia, atrioventricular block (1st -, 2nd -, 3rd degree), junctional rhythms, intraventricular conduction delays, decreased cardiac contractility, hypotension, cardiac failure (including cardiogenic shock), cardiac arrest/asystole, and pulseless electrical activity.
•
Central nervous system effects include respiratory depression, seizures, sleep and mood disturbances, fatigue, lethargy, and coma.
•
In addition, bronchospasm, mesenteric ischemia, peripheral cyanosis, hyperkalemia, and hypoglycemia (especially in children) may occur.
10.2 Treatment Recommendations
Because of its approximately 9-minute elimination half-life, the first step in the management of toxicity should be to discontinue the esmolol hydrochloride infusion. Then, based on the observed clinical effects, consider the following general measures.
Bradycardia
Consider intravenous administration of atropine or another anticholinergic drug or cardiac pacing.
Cardiac Failure
Consider intravenous administration of a diuretic or digitalis glycoside. In shock resulting from inadequate cardiac contractility, consider intravenous administration of dopamine, dobutamine, isoproterenol, or inamrinone. Glucagon has been reported to be useful.
Symptomatic Hypotension
Consider intravenous administration of fluids or vasopressor agents such as dopamine or norepinephrine.
Bronchospasm
Consider intravenous administration of a beta2 stimulating agent or a theophylline derivative.
10.3 Dilution Errors
Massive accidental overdoses of esmolol hydrochloride injection have resulted from dilution errors. Some of these overdoses have been fatal while others resulted in permanent disability. Bolus doses in the range of 625 mg to 2.5 g (12.5-50 mg/kg) have been fatal. Patients have recovered completely from overdoses as high as 1.75 g given over one minute or doses of 7.5 g given over one hour for cardiovascular surgery. The patients who survived appear to be those whose circulation could be supported until the effects of esmolol hydrochloride injection resolved.
DESCRIPTION SECTION
11 DESCRIPTION
Esmolol hydrochloride injection is a beta adrenergic receptor blocker with a very short duration of action (elimination half-life is approximately 9 minutes). Esmolol hydrochloride is:
•
(±)-Methyl p-[2-hydroxy-3-(isopropylamino) propoxy] hydrocinnamate hydrochloride and has the following structure:
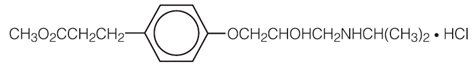
•
Esmolol hydrochloride has the molecular formula C16H26NO4Cl and a molecular weight of 331.8. It has one asymmetric center and exists as an enantiomeric pair.
•
Esmolol hydrochloride, USP is a white to off-white crystalline powder. It is a relatively hydrophilic compound which is very soluble in water and freely soluble in alcohol. Its partition coefficient (octanol/water) at pH 7.0 is 0.42 compared to 17.0 for propranolol.
11.1 Esmolol Hydrochloride Injection Dosage Forms
Esmolol hydrochloride injection is a clear, colorless to light yellow, sterile, nonpyrogenic solution of esmolol hydrochloride. The formulation for esmolol hydrochloride injection is described in the table below:
Table 4: Esmolol Hydrochloride Injection Formulation|
Q.S. = Quantity sufficient | |
|
Esmolol Hydrochloride Injection | |
|
Esmolol Hydrochloride, USP |
10 mg/mL |
|
Water for Injection, USP |
Q.S. to volume of 10 mL |
|
Sodium Acetate Anhydrous, USP |
1.688 mg/mL (equivalent to 2.8 mg/mL Sodium Acetate Trihydrate) |
|
Glacial Acetic Acid, USP |
0.546 mg/mL |
|
Sodium Hydroxide |
Q.S. to adjust pH to 4.5 to 5.5 |
|
Hydrochloric Acid |
Q.S. to adjust pH to 4.5 to 5.5 |
INFORMATION FOR PATIENTS SECTION
17 PATIENT COUNSELING INFORMATION
Physicians should inform patients of the risks associated with esmolol hydrochloride injection:
•
The most common adverse reactions are symptomatic hypotension (hyperhidrosis, dizziness) and asymptomatic hypotension.
•
Inform patients or caregivers that there is a risk of hypoglycemia when esmolol is given to patients who are fasting or who are vomiting. Monitor for symptoms of hypoglycemia [see Warnings and Precautions (5.6)].
Manufactured for:
Mylan Institutional LLC
****Morgantown, WV 26505 U.S.A.
Manufactured by:
Mylan Institutional
****Galway, Ireland
50103382
Revised: 2/2025
MI:ESMOIJ:R6
HOW SUPPLIED SECTION
16 HOW SUPPLIED/STORAGE AND HANDLING
16.1 How Supplied
Esmolol Hydrochloride Injection, 100 mg/10 mL (10 mg/mL) is supplied as:
NDC 67457-182-10
carton containing 10 x 10 mL single-dose vials
16.2 Storage
Store at 20° to 25°C (68° to 77°F). [See USP Controlled Room Temperature.] Protect from freezing. Avoid excessive heat.
Discard unused portion.
